Drug and alcohol addiction severely damages your essential organs through multiple pathways. Your brain’s neural circuits become disrupted, reducing cognitive function by 30-40%. Your heart faces dangerous arrhythmias and structural changes, while your liver’s detoxification abilities deteriorate, leading to cirrhosis. Your lungs experience increased disease susceptibility and tissue damage, and your kidneys risk failure from recurring injuries. Understanding these specific organ impacts can guide critical intervention decisions.
Understanding the Impact on Brain Function and Mental Health

While addiction is often viewed as a matter of willpower, scientific evidence reveals it as a complex brain disorder that systematically disrupts neural circuits and cognitive function. Your brain’s reward system becomes overstimulated, leading to compulsive drug-seeking behavior and decreased baseline dopamine levels. The overwhelming dopamine surges from substances can be up to ten times stronger than natural rewards.
You’ll experience significant structural changes, including reduced gray matter in your prefrontal cortex and hippocampus, resulting in cognitive flexibility deficits and impaired decision-making. These alterations affect your ability to form memories, maintain attention, and process sensory information effectively. Research shows that with sustained brain recovery, cognitive function can significantly improve after 14 months of abstinence. Sensory processing impairments can manifest alongside emotional dysregulation and decreased impulse control. Long-term substance abuse can trigger seizures and tremors during withdrawal, particularly when stopping alcohol or benzodiazepine use.
The neuroplastic changes in your brain create persistent drug-seeking pathways while weakening self-regulatory circuits. This rewiring can reduce your cognitive function by 30-40% compared to non-users, affecting your ability to learn new skills and manage stress effectively.
Effects on the Cardiovascular System and Heart Health
Since substance addiction severely impacts cardiovascular function, you’ll face significant risks to your heart health through both acute and chronic mechanisms. During acute overdose events, your heart can experience dangerous arrhythmias, sudden blood pressure spikes, and reduced oxygen flow with cocaine increasing heart attack risk sevenfold. Marijuana use can cause elevated heart rate and blood pressure in the short term, though its long-term cardiovascular effects remain unclear.
Chronic use leads to progressive deterioration, with alcohol contributing to 65% of cardiovascular deaths through chronic cardiomyopathy and valve damage. Your heart faces additional threats from opioids (13.7% of deaths) and cocaine (9.8% of deaths) through chronic inflammation and structural changes. Women and rural-area residents have seen a notable rise in cardiovascular deaths associated with substance use. Injection drug use further compounds these risks by introducing infection possibilities. The use of amphetamines stimulates central nerves, causing dangerous increases in heart rate and blood pressure.
If you’re using multiple substances, you’ll experience heightened dangers from their synergistic effects on your cardiovascular system.
Liver Damage and Metabolic Complications
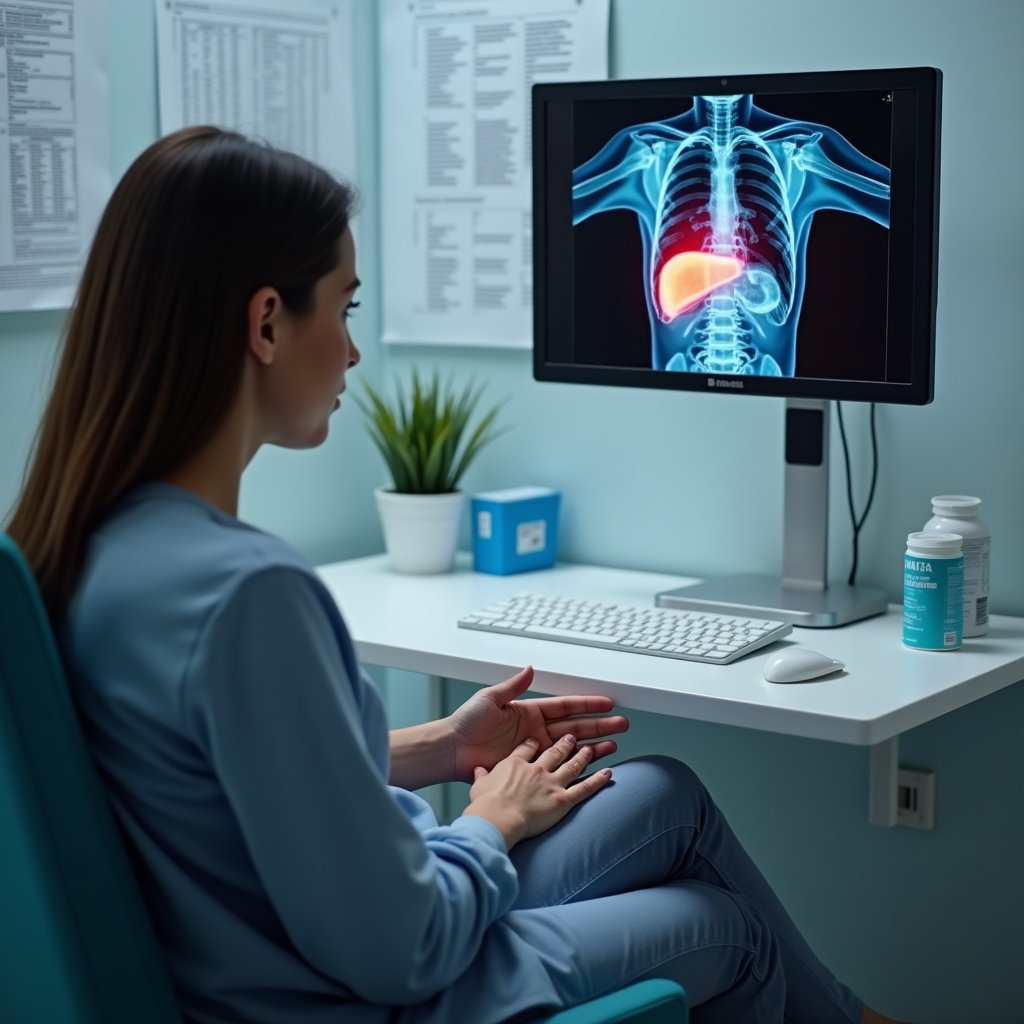
Your liver bears the brunt of substance addiction‘s destructive effects, with alcohol causing particularly severe damage to this critical organ. Heavy drinking overwhelms your liver’s detoxification capabilities, leading to a progressive cascade of complications from fatty liver to potentially fatal cirrhosis. Multidisciplinary care teams are now considered essential for effectively managing alcohol-related liver disease.
Early diagnosis and complete alcohol abstinence can help reverse damage in many cases. You’ll experience nutrient absorption deficits as your liver struggles to process essential compounds and produce adequate bile for digestion. Taking common pain relievers like acetaminophen can be especially dangerous since chronic alcohol use increases your risk of liver toxicity.
The damage extends beyond basic liver function, triggering system-wide hormone dysregulation and metabolic disruptions. Your liver’s compromised ability to regulate glucose increases diabetes risk, while toxin buildup can lead to hepatic encephalopathy.
If you’re consuming more than 80g of alcohol daily, you face an 80-90% chance of developing liver abnormalities. Women are particularly vulnerable, developing damage more rapidly than men at lower intake levels.
Respiratory System Deterioration and Lung Disease
Substance addiction wreaks havoc on the respiratory system through multiple destructive mechanisms, ranging from direct tissue damage to profound alterations in breathing mechanics. You’ll face increased susceptibility to pneumonia due to compromised immune function and impaired mucociliary clearance, especially with alcohol and opioid use. Research shows that respiratory muscle strength significantly decreases in substance users compared to non-smokers.
Chronic drug exposure triggers oxidative stress induced lung injury, particularly from methamphetamine use, leading to tissue deterioration and cellular death. Cocaine users commonly experience severe black phlegm along with debilitating shortness of breath. Those with existing lung diseases face increased overdose risks when using opioids.
When you combine substances, you’re at higher risk for respiratory depression and hypoxia, which can prove lethal. If you smoke cigarettes along with opioid use as over 95% of users do you’ll experience accelerated lung damage through synergistic effects.
The resulting inflammation, repeated infections, and breathing suppression create a perfect storm for developing chronic respiratory diseases and potentially fatal complications.
Long-term Consequences for the Kidneys and Urinary System
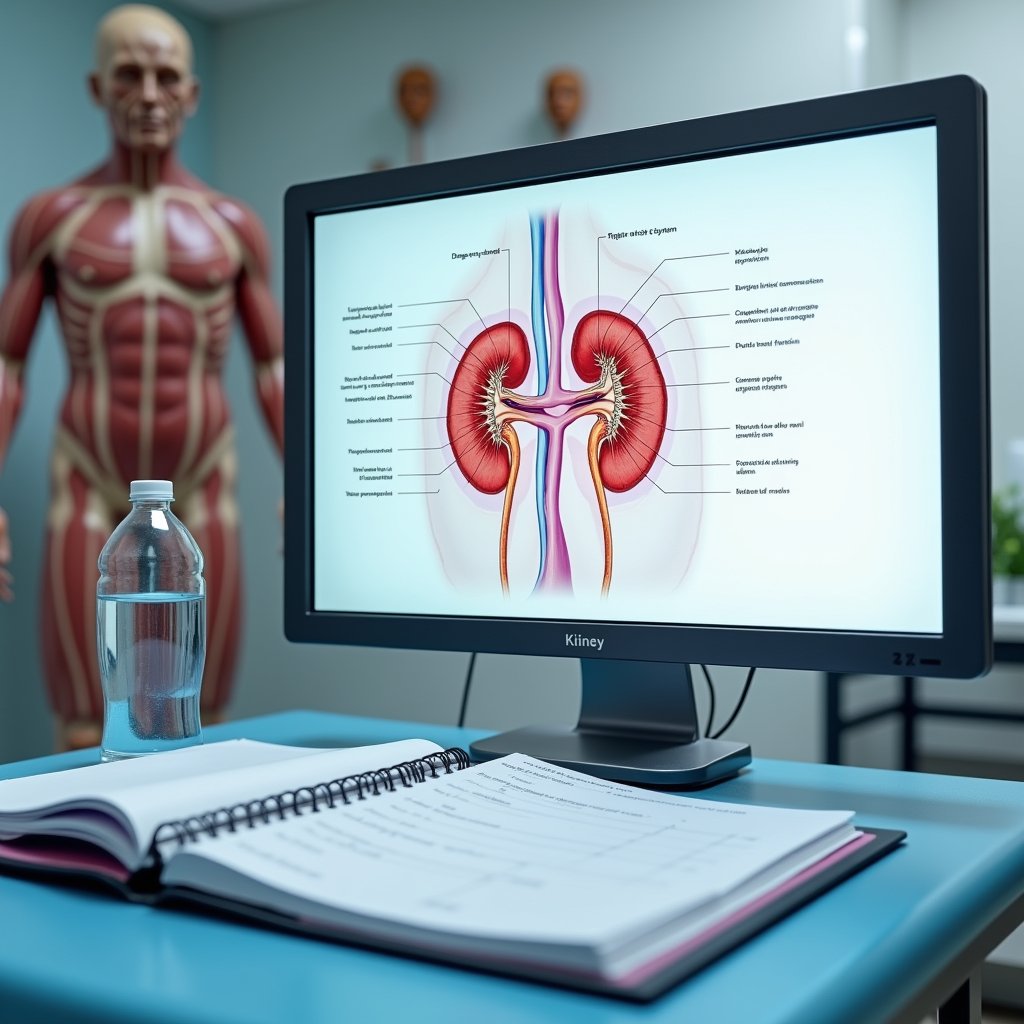
The kidneys and urinary system endure severe, progressive damage from prolonged drug and alcohol exposure, often developing alongside respiratory complications. Your kidneys’ filtration system deteriorates through multiple mechanisms: direct toxicity to renal tubules, systemic inflammation, and reduced blood flow from drug-induced vasoconstriction. Research shows that sympathetic activation typically occurs before kidney damage manifests. Chronic alcohol consumption leads to impaired fluid balance in the body, putting additional stress on kidney function.
You’ll face an increased risk of kidney stones due to chronic dehydration and concentrated urine from alcohol use. Drug-induced muscle breakdown (rhabdomyolysis) can clog kidney filters with myoglobin, while electrolyte imbalances in the urinary system disrupt essential ion regulation. Substances like cocaine can trigger renal artery dissection, severely compromising blood flow to the kidneys.
Over time, recurring acute kidney injuries lead to irreversible nephron damage and fibrotic scarring. Without intervention, you’re likely to develop end-stage renal disease, especially if you have co-existing conditions like hypertension, diabetes, or hepatitis.
Frequently Asked Questions
Can Vital Organ Damage From Addiction Be Reversed After Long-Term Recovery?
Your organ recovery potential varies drastically with long-term abstinence. Early cessation can allow partial regeneration, particularly in the liver. However, advanced damage like cirrhosis remains irreversible.
You’ll find that brain function often improves remarkably, with dopamine systems normalizing after extended sobriety. Your lungs may show limited healing capacity, while chronic respiratory damage typically persists.
Recovery success depends on your damage extent and individual health factors.
How Quickly Do Organs Begin Showing Signs of Damage From Substance Abuse?
While some organs show acute stress within hours of substance use, the timeline for significant organ deterioration varies based on the substance and abuse duration.
You’ll notice immediate effects on your brain and cardiovascular system, but lasting damage typically develops over months to years of chronic use.
Your liver may show early signs of strain within weeks, while other organ systems gradually deteriorate through sustained exposure to toxic substances.
Which Substances Cause the Most Severe and Rapid Organ Deterioration?
You’ll find that the severity and speed of organ damage largely depends on your substance abuse patterns and underlying medical conditions.
Methamphetamine and cocaine cause rapid cardiovascular deterioration within weeks of regular use. Fentanyl and other synthetic opioids can trigger immediate respiratory failure.
When you combine substances, you’ll experience accelerated multi-organ damage, with alcohol-opioid combinations being particularly destructive to your liver and kidneys within months of concurrent use.
Are Certain Organs More Resilient to Addiction-Related Damage Than Others?
Your body’s organs show varying levels of resilience to addiction-related damage based on organ vulnerability factors and individual metabolic differences.
You’ll find that your lungs and liver demonstrate remarkable regenerative abilities when you stop substance use early, while your brain’s plasticity allows for significant recovery over time.
However, your heart tends to be less resilient, as cardiovascular damage often persists even after cessation, especially with long-term stimulant or alcohol abuse.
Do Genetic Factors Influence How Addiction Affects Different Vital Organs?
Your genetic predisposition profoundly influences how addiction impacts your crucial organs. If you carry certain genetic variations in dopamine signaling genes (DRD2) or opioid receptor genes (OPRM1), you’ll likely experience more severe organ damage.
Environmental factors can trigger epigenetic changes that further modify these genetic risks. You’ll find that your liver, brain, and cardiovascular system may respond differently to substance use based on your unique genetic profile.





