Alcohol directly damages your brain by disrupting neural communication pathways and killing brain cells through oxidative stress. You’ll experience immediate effects like impaired cognition and motor skills within 1-2 drinks, while long-term heavy drinking leads to cerebral atrophy, memory loss, and permanent damage to critical regions like the hippocampus and prefrontal cortex. Women and older adults face accelerated deterioration patterns. Understanding the full scope of alcohol’s neurotoxic effects reveals even more concerning implications for brain health.
The Immediate Impact of Alcohol on Brain Function
When alcohol enters your bloodstream, it rapidly disrupts the brain’s neural communication pathways, triggering a cascade of cognitive and behavioral impairments. You’ll experience slowed mental processing within 1-2 drinks, as alcohol interferes with your brain’s information-processing abilities and neurotransmitter function. Alcohol’s neurotoxic properties can lead to intellectual deficits that worsen with repeated exposure.
Your impaired motor coordination becomes evident through slurred speech and unsteady gait, while your vision and hearing may blur due to disrupted sensory processing. The alcohol suppresses GABA activity and alters glutamate levels, affecting your judgment and decision-making capabilities. You’ll notice reduced inhibitory control and increased risk-taking behavior as your prefrontal cortex function diminishes. Short-term memory formation becomes compromised, making it difficult to recall recent events. Alcohol reaches your brain in within five minutes of consumption, causing immediate effects on cognitive function. Continued heavy drinking can result in alcohol poisoning, a severe and potentially life-threatening condition.
These effects intensify with continued consumption, potentially leading to severe central nervous system depression.
Understanding Long-Term Brain Deterioration
Your brain’s structural integrity progressively deteriorates through chronic alcohol exposure, with visible cerebral atrophy and widespread neuron loss affecting multiple regions, particularly the frontal lobe and cerebellum. Thiamine deficiency from chronic alcohol use can lead to permanent lesions in the diencephalon region.
The brain’s automatic functions weaken as alcohol impacts the medulla, leading to dangerous disruptions in breathing, heart rate, and blood pressure regulation. You’ll experience increasingly severe cognitive deficits, including memory problems, reduced planning capacity, and impaired decision-making abilities as the damage accumulates over time. However, unlike typical dementia, these cognitive impairments may show partial recovery if alcohol consumption is stopped.
Through interactions with malnutrition and potential head injuries, you’re at heightened risk for developing serious neurological conditions, including Wernicke-Korsakoff syndrome and early-onset dementia.
Progressive Neurological Damage Patterns
The progressive deterioration of brain tissue from chronic alcohol exposure follows distinct anatomical and functional patterns, affecting multiple neural systems with varying degrees of severity. You’ll notice cerebellum degeneration manifests through compromised motor coordination, while basal ganglia damage disrupts reward processing and perpetuates addictive behaviors.
| Brain Region | Primary Impact | Functional Deficit |
|---|---|---|
| Prefrontal Cortex | Dopamine Disruption | Impaired Decision-Making |
| Hippocampus | Volume Loss | Memory Deterioration |
| Cerebellum | Neural Death | Motor Dysfunction |
| Limbic System | Circuit Disruption | Mood Dysregulation |
The severity of deterioration correlates directly with your lifetime alcohol consumption. Women experience accelerated damage due to physiological differences, while older adults show heightened vulnerability. Binge drinking patterns (≥0.08% BAC) accelerate structural damage, particularly affecting white matter integrity and cellular architecture through oxidative stress and neuronal death.
Memory Loss and Dementia
Building upon the patterns of progressive brain damage, long-term alcohol consumption profoundly shapes dementia risk through complex dose-dependent relationships. You’ll find that sustained heavy drinking (>14 units/week) triggers structural shrinkage in memory-critical brain regions, while moderate consumption paradoxically shows protective effects against Alzheimer’s compared to abstinence. Those who maintain mild to moderate drinking show decreased risk of developing dementia compared to non-drinkers. Excessive alcohol intake leads to a lack of thiamine that can severely impact brain function. Recent research reveals a linear relationship between alcohol consumption and dementia risk.
Social determinants of alcohol-related dementia vary globally, with about 10% of cases directly linked to alcohol use, rising to 20% in young-onset cases. Genetics and environmental influences on alcohol neurotoxicity play essential roles, particularly when interacting with existing health conditions. You’re at heightened risk if you’ve had alcohol-related hospitalizations or sudden changes in drinking patterns. The damage manifests through impaired neuroplasticity and atrophy in hippocampal and prefrontal regions, fundamentally disrupting memory formation and cognitive function.
Critical Brain Regions Vulnerable to Alcohol
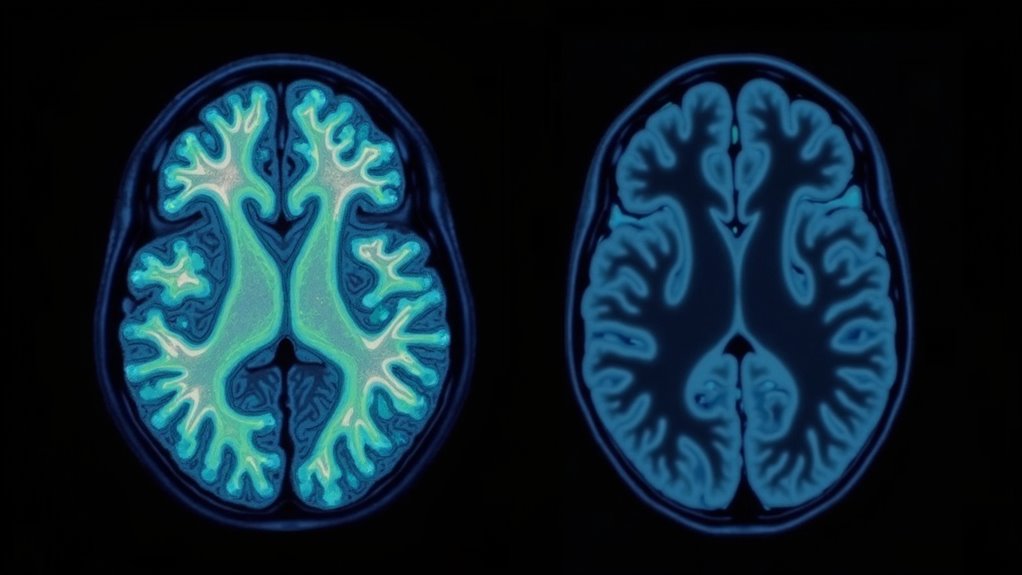
Your brain’s memory center, the hippocampus, experiences significant deterioration from prolonged alcohol exposure, leading to profound deficits in both short-term and long-term memory formation.
Research reveals that the dorsomedial striatum activity remains impaired for months after alcohol withdrawal. The prefrontal cortex, responsible for executive functions like decision-making and impulse control, shows marked vulnerability to alcohol’s neurotoxic effects. The cerebellum and balance are severely compromised in chronic alcoholics, making it difficult to maintain postural stability even when sober. These critical regions’ concurrent degradation creates a devastating impact on your cognitive abilities, as you’ll struggle with both forming new memories and exercising sound judgment in daily activities.
Hippocampus and Memory Loss
While many brain regions suffer from alcohol’s toxic effects, chronic alcohol consumption particularly devastates the hippocampus, a critical structure for learning and memory formation. You’ll experience memory consolidation issues and increased risk of alcohol-related seizures as this fundamental brain region shrinks. Using advanced multimodal MRI scanning, researchers can precisely measure and track alcohol-induced hippocampal deterioration. Women achieve higher blood alcohol levels compared to men when consuming the same amount of alcohol. When blood alcohol concentration reaches 0.16 percent, blackouts frequently occur as hippocampal function becomes severely impaired.
| Impact Area | Men | Women |
|---|---|---|
| Location | Right hippocampus | Bilateral damage |
| Onset | Earlier drinking | Later onset |
| Volume Loss | Global shrinkage | Greater vulnerability |
Your hippocampus shows distinct gender-based vulnerabilities, with women experiencing bilateral volume deficits despite later onset of heavy drinking. MRI studies reveal that chronic alcohol use triggers proportional brain shrinkage, where hippocampal tissue loss correlates with comprehensive brain volume reduction. Your risk increases with early-onset drinking and higher lifetime consumption, though genetic factors can influence your individual susceptibility to this damage.
Prefrontal Executive Function Decline
Three critical executive functions deteriorate when alcohol chronically affects your prefrontal cortex: inhibitory control, decision-making capacity, and emotional regulation. Your brain’s executive function maturation becomes severely disrupted, particularly if you’re an adolescent engaging in binge drinking. You’ll experience progressive impairment of your ability to multitask and plan effectively, while emotional regulation impairment manifests through weakened prefrontal-limbic connectivity.
Even moderate drinking compromises your inhibitory control before other cognitive deficits become apparent. Studies show that brain compensatory mechanisms help maintain normal performance in younger binge drinkers, but this protection diminishes over time. While you might perform adequately on standardized tests initially, you’ll notice difficulties in real-world functioning as dysexecutive symptoms emerge. The damage becomes permanent with continued exposure, leading to prefrontal cortex atrophy and increased risk of neurodegenerative conditions. Early intervention is essential, as complete recovery requires abstinence and may remain limited in chronic cases.
Common Neurological Disorders Linked to Drinking
Chronic alcohol consumption can trigger several devastating neurological disorders that progressively damage the brain and nervous system. You’ll notice distinct cerebral atrophy patterns and alcoholic psychosis symptoms across conditions like Wernicke-Korsakoff Syndrome, which develops in two phases and causes severe memory loss and confusion.
Alcoholic neuropathy affects your peripheral nerves, leading to numbness and muscle weakness in up to 66% of chronic cases.
You’re also at risk for alcoholic dementia, causing cognitive decline and poor coordination, while alcoholic cerebellar degeneration impairs your motor skills and speech. Heavy drinking can trigger strokes through blood pressure fluctuations and coagulation disorders.
While early intervention with alcohol cessation and thiamine supplementation may help, these conditions often cause permanent damage if left untreated.
How Alcohol Destroys Brain Cells
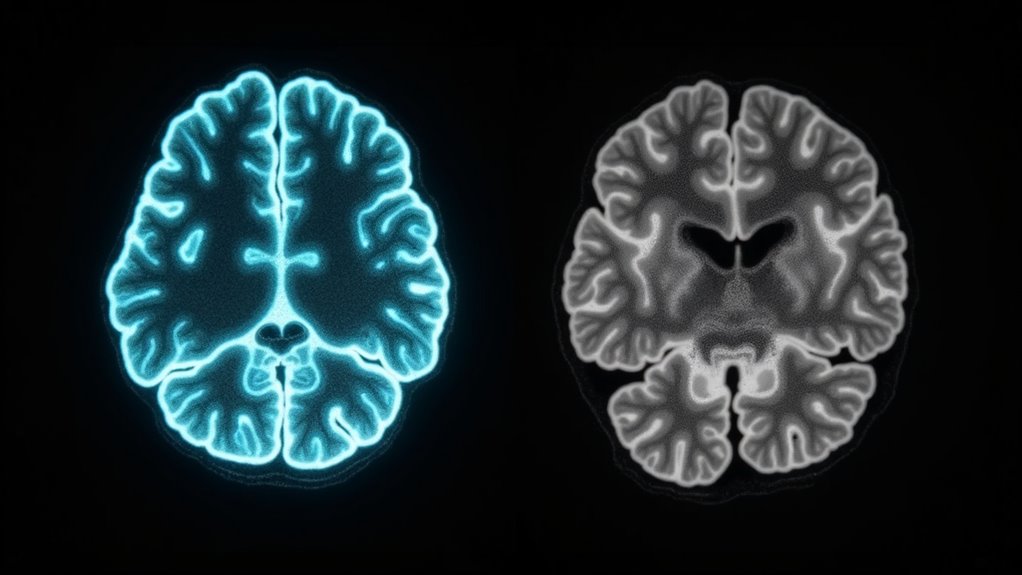
Through multiple destructive mechanisms, alcohol inflicts severe damage on your brain’s cellular architecture. When you drink, alcohol disrupts essential cellular communication pathways, directly killing neurons while triggering molecular mechanisms of oxidative stress.
Your brain cells face assault from toxic metabolites like acetaldehyde, while impaired glucose metabolism accelerates cellular deterioration.
Alcohol-induced inflammation and neurodegeneration manifest through several pathways. You’ll experience reduced hippocampal neurogenesis by up to 40% during binge drinking episodes, as alcohol blocks neural stem cell proliferation.
The damage extends to your blood vessels, compromising nutrient delivery and oxygen flow to brain tissues. In addition, you’ll develop thiamine deficiency, leading to severe enzymatic disruptions. These combined effects result in widespread brain tissue shrinkage, particularly affecting your cerebellum and cognitive centers.
Risk Factors for Alcohol-Related Brain Damage
While alcohol’s direct cellular damage presents immediate concerns, specific risk factors considerably amplify your vulnerability to alcohol-related brain damage (ARBD). Your genetic susceptibility, gender, and maturity combine with drinking patterns to determine risk levels. If you’re male and over 45, you face heightened ARBD risks, particularly when engaging in binge drinking or prolonged heavy consumption.
Nutritional deficits play a pivotal role, as alcohol disrupts your body’s ability to absorb and process essential nutrients, especially thiamine. Your cardiovascular health drastically impacts ARBD development through reduced blood flow and oxygen delivery to brain tissue. Supplementary risk factors include concurrent substance use, repeated head injuries from alcohol-related accidents, and unidentified biological vulnerabilities that explain why some heavy drinkers develop ARBD while others don’t.
Medical Complications and Brain Health
Alcohol’s devastating effects on brain health manifest through multiple interrelated medical complications, ranging from structural damage to severe cognitive deficits. You’ll find the mental health implications extend far beyond acute intoxication, creating substantial societal costs through long-term disability and healthcare burden.
Key medical complications that directly impact your brain health include:
- Widespread neuronal death and reduced synaptic connections, particularly in areas controlling decision-making
- Development of Wernicke-Korsakoff syndrome due to severe thiamine deficiency
- Autonomic nervous system dysfunction leading to multiple organ system failures
- Progressive cognitive decline that can persist even after achieving sobriety
The compounding effects of malnutrition, liver disease, and direct neurotoxicity create a complex web of damage that’s often irreversible without early intervention and sustained abstinence.
Recovery and Brain Healing After Alcohol Use
Recent scientific evidence demonstrates that the brain can heal considerably after alcohol cessation, though the recovery trajectory varies considerably among individuals. You’ll notice primary signs of cognitive improvement within the initial two weeks of sobriety, with more substantial structural changes occurring over weeks to months.
Your brain’s healing process depends on several key factors influencing recovery, including the duration and severity of alcohol abuse, your baseline health status, and the presence of co-occurring conditions.
While the recovery timeline can extend over years, you’ll experience progressive improvements in brain function through neuroplasticity and neurogenesis. Your hippocampus begins repairing itself early in recovery, though complete neural pathway reconstruction requires sustained abstinence.
Supporting this healing process through professional treatment, proper nutrition, and lifestyle modifications enhances your recovery outcomes.
Prevention Strategies and Treatment Options
Building on the brain’s natural healing capabilities, effective prevention and treatment strategies can substantially reduce alcohol-related neural damage. Implementing behavioral communication strategies requires maintaining open body language while avoiding confrontational interactions. Policy-based prevention strategies focus on establishing clear protocols for treatment and recovery.
Key approaches include:
- Avoid personalizing negative behaviors and maintain non-judgmental communication during treatment sessions
- Use evidence-based interventions that focus on positive reinforcement rather than punitive measures
- Establish consistent behavioral protocols that promote engagement in dedicated long-term rehabilitation
- Implement therapeutic communication techniques that ignore provocative comments while encouraging constructive dialogue
These strategies create an environment conducive to neural recovery while addressing both immediate and long-term treatment needs for alcohol-related brain damage.
Frequently Asked Questions
Can Brain Damage From Alcohol Affect a Person’s Personality Permanently?
Yes, you’ll experience permanent personality changes when your brain sustains significant damage. Your impaired cognitive abilities can fundamentally alter how you think, feel, and behave.
You’ll notice shifts in emotional regulation, decision-making, and impulse control that may persist even after recovery. These changes often become permanent features of your personality, and you’ll face an increased risk of dementia as these alterations continue to impact your brain’s structure and function.
What Role Does Genetics Play in Alcohol-Related Brain Damage?
Your genetic predisposition plays a vital role in how your brain responds to alcohol exposure. If you’re genetically susceptible, your brain’s immune cells (microglia) may react more aggressively, leading to accelerated synaptic damage.
Your genes can influence how rapidly you develop cognitive problems and how intensely alcohol affects your neural networks. However, it’s necessary to note that environmental factors interact with these genetic vulnerabilities to determine the overall risk.
How Does Mixing Alcohol With Other Substances Impact Brain Damage?
When you mix alcohol with other substances, you’re enormously increasing your risk of severe brain damage. The combination creates heightened neurotoxicity, as substances interact synergistically to amplify harmful effects.
Your brain experiences drastically altered neurotransmitter levels, particularly affecting GABA and serotonin systems. You’re also at greater risk for hypoxic brain injury due to respiratory depression, especially when combining alcohol with opioids or benzodiazepines.
At What Age Is the Brain Most Vulnerable to Alcohol Damage?
Your brain is most vulnerable to alcohol damage before stage 15, during critical adolescent brain development. This period features rapid growth of key structures like the prefrontal cortex and hippocampus, making them highly susceptible to alcohol exposure risks.
You’ll face the greatest potential for long-term cognitive impairment during this time, as alcohol disrupts essential neural connections and synaptic formation. Even minimal alcohol exposure can cause lasting damage to your developing brain.
Does Alcohol-Related Brain Damage Progress Differently Between Men and Women?
Yes, you’ll find significant gender differences in how alcohol-related brain damage progresses. Women experience more severe and rapid deterioration than men, even with lower alcohol consumption.
Biological factors contribute to this disparity women show higher levels of neuroinflammation, greater neuronal loss, and more pronounced brain volume reduction. They’re also more susceptible to neurotoxicity through TLR4-dependent pathways, and their hormonal fluctuations may intensify the damage during withdrawal periods.





